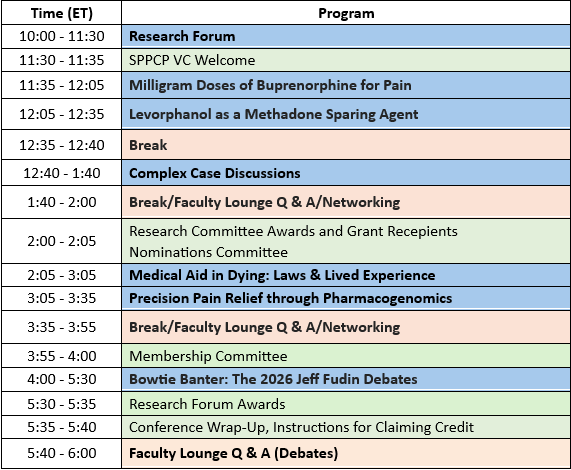
2026 Virtual Conference on Pain and Palliative Care Tuesday, May 19, 2026
|
|
Schedule (EST) |
Track 1 |
Track 2 |
Track 3 |
|
10:05 – 10:17a |
Grace Ukazim, PharmD “Evaluation of a Clinician Decision Support Alert and Prescribing Protocol on Naloxone Prescribing in High-Risk Patients” |
Selvi Chhabra, PharmD, MBA “Dose By Design: Comparing the Clinical Utility of Low-Dose and Standard Buprenorphine Induction in a Community Hospital” |
Hitomi N Iwasaki, PharmD “Transdermal Fentanyl Cost Savings in Hospice: A Retrospective Cost Analysis” |
|
10:17 – 10:29a |
Barbara Swift, PharmD, BCPS “Patient-Centered Pain Medication Optimization: Reducing High Dose Opioids in Veterans with Chronic Nonmalignant Pain” |
Katherine Mazujian, PharmD “Effectiveness of Subcutaneous Methylnaltrexone in Patients Receiving Sublingual Buprenorphine” |
Sydney Lee, PharmD “Developing a Pharmacy Resident Palliative Care Curriculum for Pharmacy Residents in a PGY2 Geriatrics Residency” |
|
10:29 – 10:41a |
Lillian Boehmer, PharmD “A Decade of Pain Stewardship: Retrospective Outcomes of a Pain PharmD Inpatient Consult Service” |
Raelyn Bitor, PharmD “Evaluation of the use of Atypical Buccal Buprenorphine Dosing for Treating Veterans with Chronic Pain in a Veterans Affairs (VA) Healthcare System” |
Hannah E McDermott, PharmD “Meperidine versus Morphine for Rigors Relief” |
|
10:41 – 10:53a |
Barbara Swift, PharmD, BCPS “Implementing Technology to Improve the Identification of Biopsychosocial Needs for Palliation of Pain in Veterans Prescribed High-Dose Opioids During Pharmacist-Led Pain Consultations” |
Kaile Allen Bernard, PharmD “Evaluation of Dronabinol Prescribing for Chronic Pain in a Veterans Healthcare Facility” |
Hitomi N Iwasaki, PharmD “Evaluation of Peak Inspiratory Flow Rate in Hospice Care Patients with Chronic Obstructive Pulmonary Disease” |
|
10:53 – 11:05a |
William J Peppard, PharmD, FCCM “Opioid-Related Emergency Department Visits (ORDEV): Design and Implementation of a Patient-centric Outcomes Measure for a Health-system Opioid Stewardship Program” |
Temple Coldren, PharmD “Impact of CYP2D6 Metabolism and CYP2D6 Inhibitor Use on Post-Procedure Pain Outcomes in Patients Prescribed Codeine or Tramadol” |
Carlton Lewis Edwards, PharmD “Opioid Dosing for Opioid-Tolerant Patients with Cancer in the Emergency Department” |
|
11:05 – 11:17a |
Aletha Loeb, PharmD “A National Comparison of Inpatient Opioid Reversal Tracking Methodologies” |
Meagan E Good, PharmD “Abdominal surgery analgesia: liposomal vs epidural bupivacaine (+/- opioids) comparison” |
|
2026 VC Program List
Milligram Doses of Buprenorphine for Pain (0.5hr – BCPMP Credit)
Taylor Butler, PharmD, BCOP
Levorphanol as a Methadone Sparing Agent (0.5hr – BCPMP Credit)
Benjamin S. Kematick, PharmD, BCPMP, BCACP
Complex Case Discussions (1 hr)
Grayson Cooley, PharmD
Diane Johnson, PharmD, BCPS, BCPMP
Grace Ukazim, PharmD
Medical Aid in Dying: Laws & Lived Experience (1hr)
Rabia Atayee, Pharm.D., BCPS, APh, FAAHPM
Lytia Jian Yin Lai, PharmD
Alban Holyoke, MD
Precision Pain Relief through Pharmacogenomics (0.5hr)
Jessica B. Emshoff, PharmD, BS, RPh, BCPS, BCGP
Bowtie Banter: The 2026 Jeff Fudin Debates (1.5 hr – BCPMP Credit)
Brooke Brodzinski, PharmD
Abby Thomas, PharmD, BCPMP
Lorin Fisher, PharmD, BCACP
Emily E. Leppien, PharmD, BCPS, BCPP
Maria Felton Lowry PharmD, BCPS, BCGP
Jessica Geiger PharmD, MS, BCPS
Live Meeting Schedule
Presentation Faculty, Descriptions, and Learning Objectives
See speaker bios here!
|
Title: |
Milligram Doses of Buprenorphine for Pain |
|
Faculty: |
Taylor Butler, PharmD, BCOP |
|
CE Credits |
0.5 hr live CE |
|
Course |
This continuing pharmacy education activity will address the expanding role of buprenorphine milligram dosing in pain management. The program will review current evidence regarding buprenorphine milligram dosing strategies and formulation selection when used for pain. Emphasis will be placed on pharmacist driven assessment, safety monitoring, and interdisciplinary collaboration to optimize patient centered pain control. |
|
Learning |
|
|
Title: |
Levorphanol as a Methadone Sparing Agent |
|
Faculty: |
Benjamin S. Kematick, PharmD, BCPMP, BCACP |
|
CE Credits |
0.5 hr live CE |
|
Course |
Most palliative care practitioners may be aware of the potential utility of levorphanol, and may have even used it in patients based on positive data in recent RCTs. However using it regularly can be difficult due to costs and access, with a relatively more familiar and cheaper alternative (methadone) available. 2Occasionally patients may not be able to continue on methadone therapy due to cardiotoxicity and alternatives need to be considered. Using rational polypharmacy may allow for a more practical way to help patients by taking advantage of the beneficial properties of levorphanol (limited QT prolongation), and methadone (cheap and accessible). |
|
Learning |
|
|
Title: |
Complex Case Discussions 2026 |
|
Faculty: |
Grayson Cooley, PharmD |
|
CE Credits |
1 hour live CE |
|
Course |
This program will examine real-world cases to address the challenges of managing complex cancer pain. Through patient case discussions, participants will explore evidence-based treatment strategies in complex cases, including the role of lidocaine infusions, approaches to severe bone pain, and the importance of shared decision-making. By integrating clinical expertise with patient-centered care, this session will equip providers with practical tools to optimize pain management in complex cancer pain. |
|
Learning |
|
|
Title: |
Medical Aid in Dying: Laws & Lived Experience |
|
Faculty: |
Rabia Atayee, Pharm.D., BCPS, APh, FAAHPM |
|
CE Credits |
1 hour live CE |
|
Course |
Medical Aid in Dying (MAID) is increasingly important in palliative and end‑of‑life care as more U.S. states adopt legislation allowing patients at end-of-life who meet the state legislation requirements to request a medication regimen to hasten death. Pharmacists play a critical role in ensuring safe, ethical, and patient‑centered access to MAID, particularly in states with established programs. This session will provide an overview of MAID laws across the United States, with deeper clinical and logistical insight from two practicing pain and palliative care pharmacists with experience in California and Washington’s MAID processes. Participants will gain a working understanding of legal frameworks, clinical eligibility criteria, medication regimens, pharmacy logistics, and clinical cases that highlight the lived experiences of patients and caregivers. Ethical considerations, communication strategies, and approaches to interdisciplinary collaboration will also be discussed. |
|
Learning |
|
|
Title: |
Precision Pain Relief through Pharmacogenomics |
|
Faculty: |
Jessica B. Emshoff, PharmD, BS, RPh, BCPS, BCGP |
|
CE Credits |
0.5 hour live CE |
|
Course |
This presentation will explore how genetic variations influence individual responses to opioid analgesics. Delving into the science of pharmacogenomics, it will highlight how genes affect opioid metabolism, efficacy, and risk of adverse effects. The session will cover key genetic markers, such as CYP2D6 and OPRM1, and their role in crafting personalized treatment plans and understanding response to therapy. Attendees will learn about current research, clinical applications, and challenges in implementing pharmacogenomic testing in pain management. |
|
Learning |
|
|
Title: |
Bowtie Banter: The 2026 Jeff Fudin Debates |
|
Faculty: |
Brooke Brodzinski, PharmD |
|
CE Credits |
1.5 hours live CE |
|
Course |
The Jeff Fudin Debates carry on a long-standing tradition of clinical debates in pain, hospice and palliative care. There are many controversial topics in this area of practice, and these debates will delve into the evidence on both sides of each topic. The issues debated will focus on pain management, palliative care, and hospice topics of interest to healthcare practitioners who care for these patients. Debates this year include the use of suzetrigine for pain, gabapentin for pain, and the use of ketamine for refractory end of life symptoms. |
|
Learning |
|
 Accreditation is provided by The American Pharmacists Association. The American Pharmacists Association is accredited by the Accreditation Council for Pharmacy Education.
Accreditation is provided by The American Pharmacists Association. The American Pharmacists Association is accredited by the Accreditation Council for Pharmacy Education.
 Programs are accredited for continuing education through a partnership with the American Pharmacists Association (APhA).
Programs are accredited for continuing education through a partnership with the American Pharmacists Association (APhA).